NAHQ CPHQ - Certified Professional in Healthcare Quality Examination
The most important determinant of quality improvement success is
Data from an Incident reporting system compares Incident rates for one facility to similar facilities:
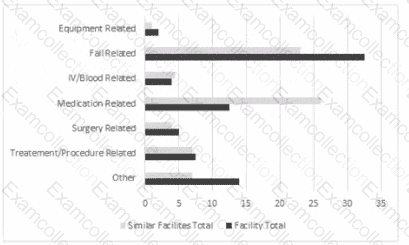
After reviewing the graph, which of the following should be done first?
A surgeon has a surgical site infection rate of 6.7% for a particular procedure. The average infection rate for other surgeons performing the same procedure at this facility is 3.3%. After notifying the department chair of this situation, the quality professional should recommend
Which of the following led to large data sets being available to healthcare quality professionals?
Six months after implementing a new cardiac rehabilitation program, an organization notes many patients that meet criteria are not enrolled. Which of the following is the most effective strategy to increase the enrollment rate?
Which of the following is the strongest intervention for preventing medication safety events?
The upper and lower limits of a control chart are
Another organization has requested data and outcomes related to a specific medical staff provider. What is the most appropriate action?
Which of the following best describes the technique of assessing the current level of performance and comparing it to the desired level of performance?
There has been an increase in readmissions and chart reviews show that it is related to medication non-adherence post-discharge. To improve medication adherence, the quality professional recommends staff:
A hospital’s Quality Council has prioritized four quality improvement initiatives using the following matrix:
Quality Improvement Initiative
Relation to Strategic Plan
Overall Positive Patient Impact
Degree of Risk to Patient
Reduce patient falls by 10%
100
20
60
Reduce wrong-site surgeries to zero
90
60
90
Reduce medication dispensing time by 20%
90
80
30
Reduce central line infections by 30%
40
90
90
Which initiative should be the highest priority?
Each provider in a primary care practice has the potential to earn a $20,000 bonus based on individual performance on select Healthcare Effectiveness Data and Information Set (HEDIS) indicators, as outlined below:
Percent of Bonus Earned
Indicator
Performance Target (met if ≥ target)
25%
Breast Cancer Screening (BCS)
74%
25%
Controlling High Blood Pressure (CBP)
72%
50%
Childhood Immunization Status (CIS)
63%
Provider performance is as follows:
Provider
BCS
CBP
CIS
A
75%
71%
63%
B
77%
69%
65%
C
79%
73%
64%
D
73%
74%
62%
Based on this information, which of the following conclusions is accurate?
A national health plan has recently acquired a local health plan. At the year anniversary of the merger, the -local health plan staff still struggles with the transition to the new organizational values. Which of the following Is the most likely explanation for the difficulty?
What is the best method to communicate detailed patient experience scores?
Which of the following is the best disease management approach to reduce hospitalizations for patients with high blood pressure?



